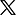Unconventional Covid-19 treatment saves lives at Tygerberg Hospital



Photo by Damien Schumann
Dr Usha Lalla (left) and Dr Coenie Koegelenberg (right).
Photo by Damien Schumann
In the midst of the Covid-19 pandemic, doctors at Tygerberg Hospital implemented a daring, lesser-known treatment that not only bypassed the imminent ventilator shortage caused by the large number of critically ill patients, but potentially saved thousands of lives, while also providing a more patient-friendly experience.
In a research article published this week in The Lancet’s EClinicalMedicine, medical experts from Stellenbosch University (SU) and the University of Cape Town (UCT) described how they were able to successfully treat half of all their critically ill Covid-19 patients by using high-flow nasal oxygen (HFNO) and avoiding mechanical ventilation.
HFNO is a non-invasive oxygen therapy that channels oxygen into the lungs through nasal tubes at a high flow rate – up to 60 litres a minute. HFNO is considered to be gentler on patients than mechanical ventilation and allows patients to eat, talk and engage with others in the ward.
Ventilation, on the other hand, is considered an invasive treatment that requires a tube to be inserted into the patient’s airway, which can cause severe discomfort and necessitates sedation in some patients.
When the first Covid-19 patients with acute respiratory distress were admitted to Tygerberg Hospital’s intensive care unit (ICU) in March, doctors treated them according to the internationally recommended regimen of mechanical ventilation.
In line with international trends, there were high mortality rates among ventilated patients.
The first seven patients all received ventilation and unfortunately all of them died, Covid-19 ICU manager Dr Usha Lalla recalled.
Lalla is also an internal medicine specialist with SU’s Faculty of Medicine and Health Sciences.
At that time, a few anecdotal reports started emerging about the use of HFNO therapy in Covid-19 patients, but generally there was a reluctance to use this lesser-known treatment. Following discussions with colleagues, Lalla and the Tygerberg team tested the theory – the first patient was “up and chatting” within five days.
More patients were then treated with HFNO and the hospital achieved much higher recovery rates with this new treatment than going straight to mechanical ventilation.
News of the success of HFNO therapy quickly spread to other hospitals in the province and around the country, with other hospitals also rapidly adopting it.
This modality was also implemented at Cape Town’s Hospital of Hope where engineers had to adapt the infrastructure at short notice to accommodate the new therapy.
HFNO does not replace mechanical ventilation, which is still extensively used in the management of Covid-19 patients, but provides an additional "weapon in doctors’ arsenals" in the fight against Covid-19, SU says in a statement.
“For a resource-constrained setting in the midst of a pandemic, this had a massive impact on the management of patients,” says SU pulmonologist Professor Coenie Koegelenberg, who also works in Tygerberg Hospital’s Covid-19 ICU.
He explains that, unlike mechanical ventilation that has to be managed in the ICU, HFNO can be administered in the general ward provided that the hospital's infrastructure provides for the higher flow of oxygen that is required.
Further, it can also be safely managed by non-ICU trained doctors and nurses, saving on the country’s sparse healthcare resources.
The doctors from SU collaborated with Professor Greg Calligaro’s team at UCT to combine data of about 300 Covid-19 patients who received HFNO therapy at these facilities, with the resulting research article now considered “by far one of the biggest studies to date on HFNO”, not only in Covid-19 patients, but for any form of pneumonia.
“Our study showed that HFNO can be successfully utilised to avoid the need for mechanical ventilation in half of all patients with severe disease,” says Koegelenberg, who adds that these patients fulfilled the criteria for acute respiratory distress syndrome, and if the recommended treatment protocol was to have been followed, all would have had to be mechanically ventilated.
Comments
Press Office
Announcements
What's On
Subscribe to improve your user experience...
Option 1 (equivalent of R125 a month):
Receive a weekly copy of Creamer Media's Engineering News & Mining Weekly magazine
(print copy for those in South Africa and e-magazine for those outside of South Africa)
Receive daily email newsletters
Access to full search results
Access archive of magazine back copies
Access to Projects in Progress
Access to ONE Research Report of your choice in PDF format
Option 2 (equivalent of R375 a month):
All benefits from Option 1
PLUS
Access to Creamer Media's Research Channel Africa for ALL Research Reports, in PDF format, on various industrial and mining sectors
including Electricity; Water; Energy Transition; Hydrogen; Roads, Rail and Ports; Coal; Gold; Platinum; Battery Metals; etc.
Already a subscriber?
Forgotten your password?
Receive weekly copy of Creamer Media's Engineering News & Mining Weekly magazine (print copy for those in South Africa and e-magazine for those outside of South Africa)
➕
Recieve daily email newsletters
➕
Access to full search results
➕
Access archive of magazine back copies
➕
Access to Projects in Progress
➕
Access to ONE Research Report of your choice in PDF format
RESEARCH CHANNEL AFRICA
R4500 (equivalent of R375 a month)
SUBSCRIBEAll benefits from Option 1
➕
Access to Creamer Media's Research Channel Africa for ALL Research Reports on various industrial and mining sectors, in PDF format, including on:
Electricity
➕
Water
➕
Energy Transition
➕
Hydrogen
➕
Roads, Rail and Ports
➕
Coal
➕
Gold
➕
Platinum
➕
Battery Metals
➕
etc.
Receive all benefits from Option 1 or Option 2 delivered to numerous people at your company
➕
Multiple User names and Passwords for simultaneous log-ins
➕
Intranet integration access to all in your organisation