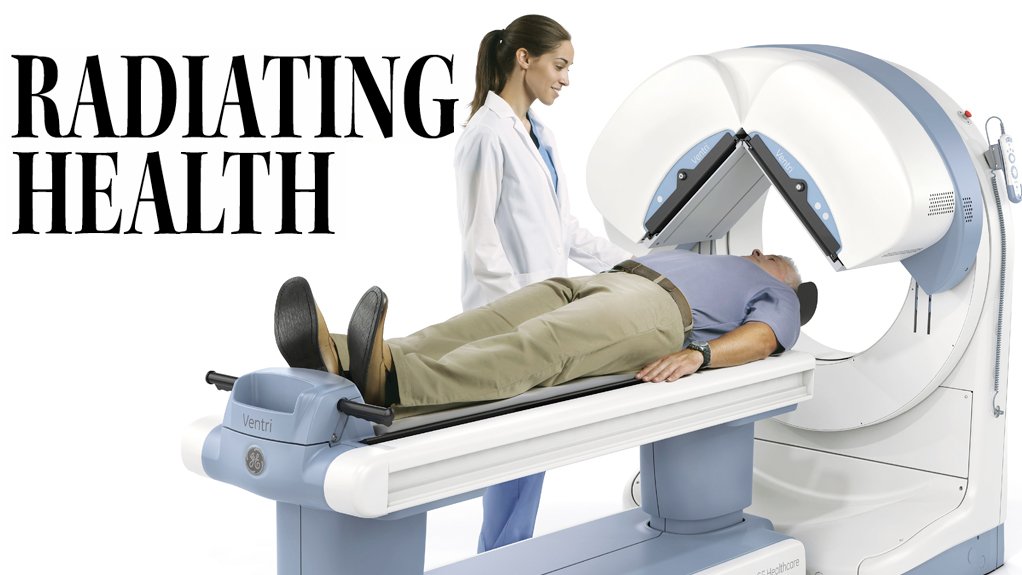
South Africa emerges as leading global nuclear medicine supplier
Nuclear medicine is defined by the Department of Medical Physics of the School of Clinical Medicine of the University of the Witwatersrand as “a speciality that makes use of radioactive tracers that emit gamma rays to assess the physiological functioning of organs and systems in the body”.
These radioactive tracers are called radio- pharmaceuticals. The US-based but international Society of Nuclear Medicine and Molecular Imaging explains: “[In] nuclear medi- cine imaging, the radiopharmaceuticals are detected by special types of cameras that work with computers to provide very precise pictures of the area of the body being imaged. Nuclear medicine can also be used to treat certain types of cancer and other diseases.” (A radioisotope is turned into a radiopharma- ceutical by linking it to peptides or other organ- specific agents; in turn, a peptide is a chemical compound containing two or more amino acids.) Nuclear medicine imaging does not, like X-rays, reveal the structure of the body; rather, it shows the functioning of the body and allows the measurement of its biological and chemical processes.
Nuclear medicine imaging uses tiny amounts of radioactive materials – the radioactive tracers or radiopharmaceuticals – which can be inhaled or swallowed by, or injected into, the patient. These radiopharmaceuticals accumulate in specific organs of the body, which are then scanned by specialist imagers linked to computers. The result is early and accurate diagnoses of conditions and diseases. The level of radiation the patient is exposed to is often lower than that received during an X-ray procedure. Radiopharmaceuticals can also be used to treat certain medical conditions. Worldwide, more than 40-million nuclear medicine diagnostic procedures are carried out each year.
Genesis
Nuclear medicine uses artificial, or manufac- tured, radioisotopes. The first artificial radioisotope was produced in 1934 by Irene Joliot-Curie and her husband Frédéric Joliot-Curie. By the end of that year, the number of such radioisotopes had increased to three. The first radioisotope used therapeutically was Phosphorus-32 by Dr John Lawrence on December 24, 1937, at the University of California, Berkeley, in the US. In December 1939, a second radioisotope joined the medical armoury, with the first use of Strontium-89, also in the US. January 1941 saw the first use of Iodine-130, also in the US. Further, Lawrence and his team started using neutron beams against cancer in 1939.
One of the consequences of the Second World War Manhattan Project, to develop the atomic bomb, was the establishment of (by previous standards) large-scale production facilities for radioisotopes. With effect from January 1, 1947, all aspects and assets of the Manhattan Project and all future military, developmental and regulatory aspects of nuclear power were subordinate to the newly established US Atomic Energy Commission (AEC – abolished in 1975), a civilian agency. Thus the AEC became responsible for the manufacture of all radioisotopes in the US. But the AEC did not market them. That was left to commercial enterprises. A company called Abbott Laboratories is believed to have been the first to market a pharmaceutical- grade radioisotope. And it was an Abbott chemist, Dr Donalee Tabern (a man, despite the name), who, in 1948, was responsible for the discovery of the first proper radiopharma- ceutical, radioiodinated human serum Albumin, marketed as RISA. The company thus became the first in the world to produce and sell radiopharmaceuticals. (The company still exists, but seems no longer to manufacture radiopharmaceuticals.)
In South Africa, nuclear medicine dates back to 1948, as well as the first importation of radioisotopes for medical purposes. Over the following years, the key equipment was also imported. Thus, in 1952, the then Pretoria General Hospital (later the HF Verwoerd Hospital and today the Steve Biko Academic Hospital) acquired a sodium iodide counter (a type of scintillation counter, an instrument invented in 1944, which measures gamma rays and low energy beta rays). In 1964, the Council for Scientific and Industrial Research (CSIR) acquired the country’s first rectilinear scanner (an instrument, invented in 1950 and now obsolete, that allowed doctors to track radioisotope tracers and radiopharmaceuticals in a patient’s body; previously geiger counters had to be used, but these lacked sensitivity). In 1969, the then HF Verwoerd Hospital obtained the country’s first gamma camera (also called the scintillation camera; invented in 1957, it does the same job as the rectilinear scanner but more rapidly, conveniently and efficiently and so has completely replaced the older instrument).
The South African Society of Nuclear Medicine was established in 1974. In 1980, the discipline became, in this country, a subspeciality under radiology before becoming a full and separate speciality in 1987. Today, seven of the national teaching hospitals have nuclear medicine departments with modern single-photon- emission computerised tomography (SPECT) gamma cameras, while most of the private hospitals in the major centres also have such departments with modern equipment. SPECT gamma cameras create three-dimensional pictures of internal organs using radioisotope tracers. Another nuclear medicine imaging technology is positron emission tomography (PET), which dates back to early experiments in the 1950s; however, in the late 1990s, PET technology was success- fully combined with computed tomography (CT) technology in a single instrument – the PET-CT scanner. South Africa also has a number of PET-CT scanners in public and private hospitals.
But that is only a part of the story. For, in 1955, the CSIR began to produce radioisotopes at its low-energy cyclotron in Pretoria. (A cyclotron is a circular type of particle accelerator; in turn, an accelerator is a device that accelerates charged particles, such as protons and electrons, to high speeds and energies.) Then, in 1965, the Safari-1 research reactor was commissioned at Pelindaba, west of Pretoria. (Safari originally stood for South African Fundamental Atomic Research Installation, but this full name has not been used for decades.) From the beginning, it produced radioisotopes. And, in 1987, the then National Accelerator Centre (since 2001, the iThemba Laboratory for Accelerator Based Sciences, or iThemba LABS), near Somerset West, in the Western Cape, started producing radioisotopes with a cyclotron. From these beginnings, South Africa has emerged as a major player in the global radioisotope market. For example, more than 20% of the nuclear medicine diagnostic procedures carried out around the world today employ radioisotopes produced by processing target materials irradiated with neutrons in Safari-1.
Health Safari
Safari-1 is operated by the South African Nuclear Energy Corporation (Necsa) and has a capacity of 20 MW. Now 49 years old, Necsa is extending its life for about ten years, but hopes to replace it with a new 15 MW to 20 MW multipurpose reactor. For many years now, one of the main functions of Safari-1 has been the production of irradiated material (known as targets) for Necsa subsidiary company NTP Radioisotopes to process for the required radioisotopes, package them and distribute to customers around the world. Despite its age, Safari-1 operates on average at full capacity for 305 days a year – a world record – and has a flawless safety and environmental protection record and impeccable operational performance. Radioisotopes produced by NTP are exported to some 60 countries on five continents.
NTP describes itself as a radiation applications business. It is focused on all business oppor- tunities related to radiation. It currently has a turnover of R1-billion and makes healthy profits. At Pelindaba, it employs more than 270 people but its total workforce, including sub- sidiaries, is some 500. It also produces radioisotopes for industrial purposes, such as nondestructive testing and process control. Currently, it manufactures the radioisotopes Molybdenum-99 (Mo-99), Iodine-131 (I-131), Iridium-192 (Ir-192) and Caesium-137 (Cs-137). Soon, it will start producing an additional radioisotope, Lutetium-177 no carrier added (Lu-177 nca) for the effective treatment of neuroendocrine cancer and for which it has obtained a manufacturing licence from German group ITG.
Each and every radioactive material has its own characteristic half-life. Half-life is the length of time taken for the radioactive material to decay to half its original radioactivity level. Half-lives can range from millionths of a second to billions of years. The half-life of Mo-99 is 66 hours, that of I-131 is about eight days, that of Ir-192 is just under 74 days and that of Cs-137 is 30 years, while Lu-177 has a half-life of 6.7 days. These differing half-lives affect what markets the products can be sold to and makes clear the need to transport radioisotopes by air. Transport of radioisotopes is in internationally-licensed containers of proven strength and structural integrity. These containers have been designed and are built by NTP. A key reason for NTP acquiring the licence to produce Lu-177 nca, which currently has to be imported from Germany, is to increase the supply of the radioisotope available to the local nuclear medicine community, increase efficiency of its use and ensure that a greater number of patients benefit from its use by eliminating the time needed to transport it from Europe.
NTP also produces radiopharmaceuticals for the local and regional markets. The process of linking a radioisotope to a peptide or other organ-specific agents to create a radiopharmaceutical is called labelling. “Currently, we import the Lu-177 and do the labelling here,” explains AEC Amersham MD Wayne Flowers. “When we start local production, we’ll still do the labelling.” Labelling is generally done in the country where the radiopharmaceuticals are to be used to ensure their maximum possible life- span. AEC Amersham is a wholly owned subsidiary of NTP and is responsible for marketing all its medical products in Africa. Sales outside of Africa are done by NTP itself.
With Lu-177 nca, for example, tumour-specific radiopharmaceuticals can now be made, to deal with neuroendocrine tumours. “This applies to both diagnosis using nuclear imaging technologies and treatment,” he explains. The tumours are treated intravenously with a radiopharmaceutical. In the case of a dotatate peptide (a dotatate is a chemical substance) linked to Lu-177, this is a highly targeted and effective therapy with minimal side effects.
However, NTP is particularly well known around the world for its production of Mo-99, which was one of its original products and which remains a very important one, with the company now holding 20% to 25% of the world market. Mo-99 serves as a precursor for the Technetium-99m (Tc-99m) radioisotope, which has a half-life of just six hours. The Tc-99m is produced in special generators and then turned into radiopharmaceuticals by being combined with organ-specific chemical compounds.
Further, Necsa was the first organisation in the world to undertake large-scale production of Mo-99 from low-enriched uranium (LEU). This milestone was achieved in December 2010, with the export of LEU Mo-99 radioisotopes, approved for medical use in the US. Previously, worldwide, all Mo-99 had been manufactured using highly-enriched uranium (HEU).
HEU can be used to manufacture nuclear weapons, but LEU cannot. In 2008, Necsa, with cooperation from the National Nuclear Security Administration (NNSA) of the US Department of Energy, converted the Safari-1 research reactor from using HEU to using LEU. Subsequently, in October 2010, the NNSA gave Necsa up to $25-million to assist in the development of Mo-99 isotopes from LEU instead of HEU. In March 2012, Belgium, France and the Netherlands – all leading producers of radio- isotopes in Europe – announced that they would follow in South Africa’s footsteps and replace HEU with LEU in the production of Mo-99. This process is expected to be completed by next year.
Life-Giving LABS
iThemba LABS manufactures radioisotopes as a secondary, although important, activity. “We are primarily a research institute,” explains iThemba LABS acting director Dr Kobus Lawrie. “Our primary mandate is research. But [radio]isotope production has grown in importance. Currently, we utilise about 30% of our beam time on isotopes – we produce them overnight during weekdays. “Initially, we supplied isotopes as a service to local hospitals, but we now export as well. Only certain isotopes can be exported – the longer lived ones. With exports, our total revenue from isotope production has grown quite substantially.”
At its Somerset West facility (iThemba LABS also has a division on the campus of the University of the Witwatersrand, in Johannesburg, but this division is not involved in the production of radioisotopes), the organisation has a 200 megaelectronvolt (MeV) cyclotron, plus an 11 MeV cyclotron that is dedicated to the production of 18-Fluorine fluorodeoxoglucose (18F FDG) radiopharmaceuticals. The manufacture of all the radioisotopes is overseen by the Radionuclide Production Department (RPD) of iThemba LABS.
Accelerators and reactors produce different kinds of radioisotopes. As a result, iThemba LABS and NTP make complementary, not competitive, ranges of products. The one product both agencies produce is 18F FDG, which is very important for the diagnosis of cancer and which has a half-life of only 110 minutes. So iThemba LABS and NTP coordinate their production and distribution of 18F FDG to ensure that every facility in the country that needs it is assured of a reliable supply.
The other radioisotopes produced for the local market are 67-Gallium Citrate and Iodine-123 products (including solutions, capsules and metaiodobenzylguanidine – MIBG). MIBG is a radiopharmaceutical used to find and diagnose certain cancers. Further, 68-Germanium/68-Gallium (68Ge/68Ga) generators are manufactured for both the domestic and export markets. (Such generators extract 68-Gallium, which emits positrons – needed for PET-CT imaging – from a decaying 68-Germanium source.) These various products are supplied to about 25 nuclear medicine facilities in South African hospitals and clinics. For the export markets, in addition to the 68Ge/68Ga generators, iThemba LABS makes 82-Strontium by irradiating rubidium metal targets (these are exported to Canada) and 22-Sodium (both as a solution and as ultrahigh-vacuum 22-Sodium positron sources).
“The production process is a combination of nuclear physics followed by radiochemical processes, then conversion of the radio- chemicals into radiopharmaceuticals,” explains RPD head Dr Clive Naidoo. “The radiopharmaceuticals are then divided into patient doses, followed by quality control processes, packaging and dispatch. The whole process involves physicists, chemists, pharmacists and electronics engineers.
“We are one of the leading suppliers of accelerator-based radioisotopes in the world market,” he reports. “With the 68-Ge/68-Ga generators we supply 40% of world demand. For Sodium-22 ultrahigh-vacuum positron sources, we are the world’s sole supplier. For Strontium-82, we meet about 27% of global demand. During the last financial year, the value of our business was about R40-million, of which 75% were exports.”
The Somerset West facility also provides proton and neutron beam therapies for treating cancers. Proton and neutron beams have different medical effects and are used to treat different tumours. “Proton beams can be tightly focused to reduce side effects,” states Lawrie. “Unfortunately, we can only treat head and neck tumours with proton beams at present, due to our setup.” Neutron beam therapy started around 1990 and proton beam therapy around 1995. Since then, some 2 000 people have been treated with neutron beams and about 500 with proton beams.
Comments
Press Office
Announcements
What's On
Subscribe to improve your user experience...
Option 1 (equivalent of R125 a month):
Receive a weekly copy of Creamer Media's Engineering News & Mining Weekly magazine
(print copy for those in South Africa and e-magazine for those outside of South Africa)
Receive daily email newsletters
Access to full search results
Access archive of magazine back copies
Access to Projects in Progress
Access to ONE Research Report of your choice in PDF format
Option 2 (equivalent of R375 a month):
All benefits from Option 1
PLUS
Access to Creamer Media's Research Channel Africa for ALL Research Reports, in PDF format, on various industrial and mining sectors
including Electricity; Water; Energy Transition; Hydrogen; Roads, Rail and Ports; Coal; Gold; Platinum; Battery Metals; etc.
Already a subscriber?
Forgotten your password?
Receive weekly copy of Creamer Media's Engineering News & Mining Weekly magazine (print copy for those in South Africa and e-magazine for those outside of South Africa)
➕
Recieve daily email newsletters
➕
Access to full search results
➕
Access archive of magazine back copies
➕
Access to Projects in Progress
➕
Access to ONE Research Report of your choice in PDF format
RESEARCH CHANNEL AFRICA
R4500 (equivalent of R375 a month)
SUBSCRIBEAll benefits from Option 1
➕
Access to Creamer Media's Research Channel Africa for ALL Research Reports on various industrial and mining sectors, in PDF format, including on:
Electricity
➕
Water
➕
Energy Transition
➕
Hydrogen
➕
Roads, Rail and Ports
➕
Coal
➕
Gold
➕
Platinum
➕
Battery Metals
➕
etc.
Receive all benefits from Option 1 or Option 2 delivered to numerous people at your company
➕
Multiple User names and Passwords for simultaneous log-ins
➕
Intranet integration access to all in your organisation